What You Need to Know About Opioid Use Disorder
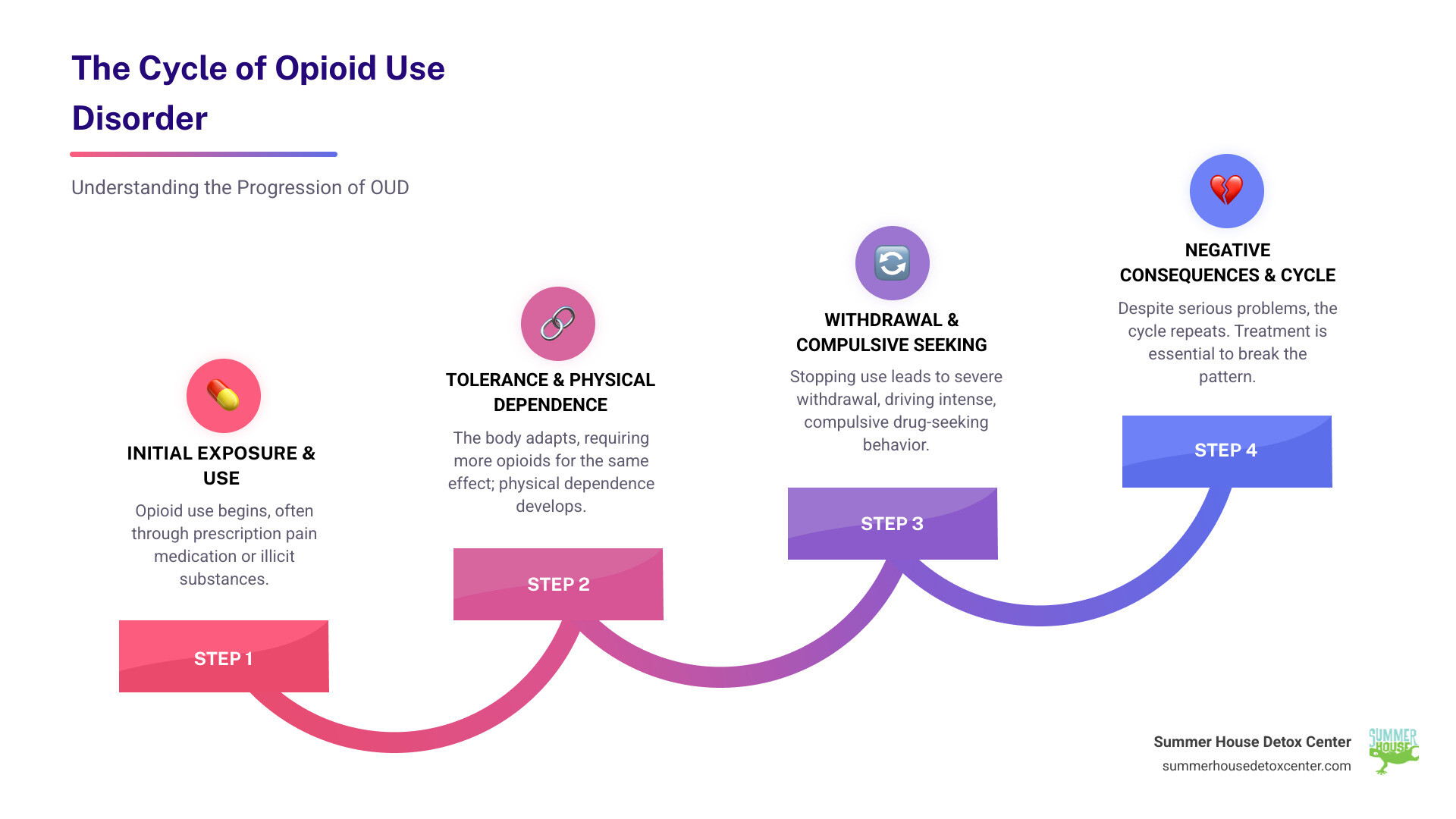
Opioid use disorder (OUD) is a treatable, chronic medical condition characterized by the compulsive use of opioids despite harmful consequences. It’s a complex brain disease, not a moral failing, and it can affect anyone, from those prescribed pain medication to individuals using illicit drugs like heroin or fentanyl.
In 2022, nearly 110,000 Americans died from drug overdoses, with over 81,000 involving opioids. Florida, including Miami-Dade County, has been hit particularly hard by this crisis, with a sharp rise in deaths linked to illicitly manufactured fentanyl, a substance 50 to 100 times more potent than morphine.
If you or a loved one is struggling, know that recovery is possible. With the right treatment, including medically supervised detox and medication-assisted treatment, people with OUD can and do reclaim their lives. This guide walks you through understanding OUD, from diagnosis to effective treatment options available in South Florida.
Common opioid use disorder vocab:
What is Opioid Use Disorder and How is it Diagnosed?
Opioid use disorder (OUD) is a medical condition defined by a problematic pattern of opioid use that causes significant impairment or distress. It’s a complex brain disease involving compulsive drug-seeking behavior, not simply a matter of physical dependence.
The diagnosis of OUD is based on criteria from the Diagnostic and Statistical Manual of Mental Disorders (DSM-5-TR). A healthcare professional will assess for at least two of eleven specific symptoms within a 12-month period. These symptoms are grouped into four main categories:
- Impaired Control: Using more opioids than intended, wanting to cut down but being unable to, spending excessive time obtaining or using opioids, and experiencing strong cravings.
- Social Impairment: Failing to fulfill major roles at work, school, or home; continuing use despite social or interpersonal problems; and giving up important activities.
- Risky Use: Using opioids in physically hazardous situations or continuing use despite knowing it’s causing physical or psychological harm.
- Pharmacological Criteria: Developing tolerance (needing more of the drug for the same effect) and experiencing withdrawal symptoms when stopping.
The severity of OUD is classified as mild (2-3 symptoms), moderate (4-5 symptoms), or severe (6 or more symptoms). Tolerance and withdrawal alone do not constitute an OUD diagnosis if the opioids are used as prescribed by a doctor.
Understanding the Symptoms and Causes
The signs of opioid use disorder are physical, behavioral, and psychological.
- Physical Symptoms: Often most noticeable during withdrawal, these include muscle aches, chills, sweating, nausea, vomiting, and insomnia.
- Behavioral Symptoms: These include taking more opioids than prescribed, trying and failing to quit, neglecting responsibilities, and engaging in risky behaviors to obtain drugs.
- Psychological Symptoms: Intense cravings, continued use despite worsening mental health, mood swings, and anxiety are common.
Several factors can increase the risk of developing OUD, including genetics, environment (like easy access to drugs), and a history of trauma or Adverse Childhood Experiences. Misusing prescription painkillers can also be a gateway to heroin or other illicit opioids.
Physical Dependence vs. Addiction
It’s crucial to distinguish between physical dependence and addiction, though they often coexist in opioid use disorder.
-
Physical Dependence: This is a natural physiological adaptation where the body gets used to the presence of a drug. If the drug is stopped abruptly, withdrawal symptoms occur. A person can be physically dependent without being addicted, especially when taking medication as prescribed.
-
Addiction (OUD): This is a chronic brain disease characterized by compulsive drug-seeking and use, despite harmful consequences. It involves changes in the brain’s reward system, making it extremely difficult to stop without professional help. Learn more about what addiction is and how it can be treated.
The Opioid Crisis: Statistics and Key Substances
The opioid crisis is a major public health emergency in the United States, with Florida being one of the most affected states. In 2022, nearly 110,000 Americans died from drug overdoses, with over 81,000 involving opioids. For local information, see Florida’s State Opioid Response Project Resources. National data is available at Overdose Death Rates.
Types of Opioids and Their Potency
Opioids vary in strength and origin:
- Natural Opioids: Derived from opium poppy (morphine, codeine)
- Semi-Synthetic: Lab-created from natural opiates (heroin, oxycodone, hydrocodone)
- Synthetic: Entirely man-made, including fentanyl and carfentanil. Carfentanil: Elephant sedative killing people
Fentanyl is 50 times more potent than heroin and 100 times more potent than morphine. See Drugs of Abuse: A DEA Resource Guide (.pdf).
The Role of Fentanyl in the Current Crisis
Fentanyl is at the heart of the modern opioid use disorder and overdose crisis in Florida. Most deaths involve illicitly manufactured fentanyl (IMF), often mixed with other drugs or pressed into counterfeit pills resembling legitimate prescriptions.
Users often don’t know they’re taking fentanyl—a tiny amount can be fatal. The DEA’s One Pill Can Kill campaign highlights this danger. The presence of xylazine in illicit fentanyl can make overdoses harder to reverse.
For those in South Florida struggling with fentanyl use, immediate help is crucial. Summer House Detox Center in Miami offers Top-rated fentanyl detox at Summer House Detox Center.
Pathways to Recovery: Effective Treatment for Opioid Use Disorder
The journey to overcome opioid use disorder is challenging, but it is unequivocally possible. The primary goals of treatment are to prevent overdose deaths, help individuals regain their health and social function, and support them in achieving long-term recovery. This requires a comprehensive, individualized approach that addresses both the physical and psychological aspects of OUD. Finding quality treatment is the first step, and resources like Finding Quality Treatment for Substance Use Disorders can guide you.
The First Step: Managing Opioid Withdrawal
For many, the fear of withdrawal is a major barrier to seeking help. Opioid withdrawal can be uncomfortable, but it’s a necessary first step in the recovery process. The symptoms can range from mild to severe, including:
- Intense cravings for opioids
- Muscle aches and bone pain
- Restlessness and insomnia
- Diarrhea, nausea, and vomiting
- Cold flashes with goosebumps (“cold turkey”)
- Involuntary leg movements
The timeline of withdrawal varies depending on the type of opioid used. For short-acting opioids like heroin, symptoms can begin within 6-12 hours of the last dose, peak around 24-72 hours, and subside within a week. For longer-acting opioids like methadone, withdrawal can start 2-3 days after the last dose and last for several weeks. You can learn more about specific symptoms and their duration at Opiate Withdrawal Symptoms.
While opioid withdrawal is rarely life-threatening on its own (unlike withdrawal from alcohol or benzodiazepines), its severity often drives individuals to continue using to avoid the excruciating discomfort. Quitting “cold turkey” without medical supervision is not only incredibly difficult but also significantly increases the risk of relapse and subsequent overdose, as tolerance decreases rapidly. This is why Why medical detox is a vital first step in recovery is so important.
At Summer House Detox Center in Miami, FL, we specialize in medically supervised detox programs, providing a safe and comfortable environment where withdrawal symptoms are managed with medication and expert care. Our dedicated Opiate Detox Center in Miami, FL helps individuals move through this challenging phase with dignity and support, setting a solid foundation for long-term recovery.
Medication-Assisted Treatment (MAT) for Opioid Use Disorder
Medication-Assisted Treatment (MAT) is considered the gold standard for treating opioid use disorder. It’s an evidence-based approach that combines FDA-approved medications with counseling and behavioral therapies. This comprehensive strategy addresses the whole person, not just the substance use. You can explore more about this approach at Medication-Assisted Treatment (MAT).
MAT medications help to:
- Normalize brain chemistry and reduce the intense physiological drive to use
- Relieve cravings that often lead to relapse
- Prevent withdrawal symptoms, allowing individuals to focus on therapy and recovery
- Block opioid effects, making it less rewarding to use illicit substances
Research shows MAT can greatly reduce the use of illicit opioids and lower the risk of overdose. For more detailed information, see How effective are medications to treat opioid use disorder?.
A significant development in expanding access to MAT occurred with the MAT Act of 2022. This legislation eliminated the DATA-Waiver (X-Waiver) program, which previously required special training for healthcare providers to prescribe buprenorphine. Now, all DEA-registered practitioners with Schedule III prescribing authority can prescribe buprenorphine for OUD, making this vital medication more accessible to individuals in need, including those in Florida.
At Summer House Detox Center, we firmly believe in the power of MAT. Our Medication-Assisted Treatment services at Summer House Detox Center in Miami are custom to each individual’s needs, providing the medical support necessary for a successful recovery journey.
FDA-Approved Medications for OUD
There are three FDA-approved medications for treating opioid use disorder, each with a distinct mechanism of action and usage protocol. We can discuss these options with you at Summer House Detox Center to determine the best fit for your recovery journey in Miami, FL.
- Methadone: A long-acting opioid agonist that prevents withdrawal and reduces cravings. It’s dispensed daily at licensed clinics. Learn more about Methadone.
- Buprenorphine (Suboxone, Subutex): A partial opioid agonist that eases withdrawal and cravings without producing a strong high. It can be prescribed by certified doctors and taken at home. Learn more about Buprenorphine.
- Naltrexone (Vivitrol): An opioid antagonist that blocks the effects of opioids. It’s not an opioid, has no potential for abuse, and is not addictive. It’s usually started after a person has fully detoxed. Learn more about Naltrexone.
Choosing the right medication depends on individual needs, medical history, and treatment goals. For a detailed comparison, see Methadone vs Suboxone: How do they differ?.
The Role of Therapy and Treatment Settings at Summer House Detox Center
Medication is a crucial component, but it’s most effective when combined with behavioral therapies and counseling. These therapies help individuals address the root causes of their addiction, develop coping skills, and build a foundation for long-term recovery.
Key Therapeutic Approaches:
- Cognitive Behavioral Therapy (CBT): Helps patients recognize and change negative thinking patterns and behaviors associated with drug use.
- Contingency Management (CM): Uses positive reinforcement to encourage abstinence.
- Motivational Interviewing (MI): Helps individuals resolve ambivalence and find the internal motivation to change.
Treatment Settings at Summer House Detox Center:
- Detoxification (Detox): The first step, providing medical supervision to manage withdrawal symptoms safely. Our Drug and alcohol detox in Miami, FL offers a supportive environment for this critical phase.
- Inpatient/Residential Detox Stay: Provides intensive, 24-hour care in a structured, comfortable environment at our Miami facility, ideal for individuals with moderate to severe OUD.
After completing detox at Summer House Detox Center, many South Florida residents continue care with community-based outpatient programs and support groups like Narcotics Anonymous, which play a vital role in maintaining recovery.
Harm Reduction, Prevention, and Support
Beyond treatment, a comprehensive approach to the opioid crisis includes harm reduction, prevention, and ongoing support—vital for saving lives and helping recovery in Florida communities.
Harm Reduction Strategies
Harm reduction minimizes negative health, social, and legal impacts of drug use:
- Naloxone Access: Making overdose-reversal drug naloxone (Narcan) widely available
- Syringe Services Programs: Providing sterile needles to reduce disease transmission
- Drug Checking: Testing services for fentanyl presence
Florida has Good Samaritan Laws protecting those who seek emergency help during overdoses.
Preventing Opioid Misuse
Key prevention strategies include:
- Safe Storage/Disposal: Secure prescription opioids and dispose properly. FDA provides a list of medicines recommended for disposal by flushing
- Patient Education: Healthcare providers should discuss opioid risks and alternatives
- Non-Opioid Pain Management: Physical therapy, acupuncture, and non-addictive medications. See Nonopioid Therapies for Pain Management
Naloxone: A Lifesaving Tool
Naloxone rapidly reverses opioid overdoses by blocking opioid effects and restoring breathing. The U.S. Surgeon General issued a public health advisory urging Americans to carry naloxone.
In Florida, naloxone is available without prescription at many pharmacies. Local health departments and community organizations in South Florida may distribute free kits with training.
Your Rights: OUD and the ADA
Opioid Use Disorder is recognized as a disability under the Americans with Disabilities Act. Individuals with OUD are protected from discrimination in employment, housing, and services. This applies to those in recovery or participating in rehabilitation programs. Employers cannot discriminate based on OUD treatment if you can perform job functions. See The Americans with Disabilities Act and the Opioid Crisis.
The Opioid Crisis: Statistics and Key Substances
The opioid crisis continues to be a profound public health challenge across the United States, including here in Florida. The numbers paint a grim picture, yet they also underscore the urgent need for effective intervention and treatment.
In 2022, nearly 110,000 Americans died from drug overdoses, with a staggering 81,000 of these deaths involving either prescription or illicit opioids. This represents a sharp increase in opioid-involved overdose deaths over a decade, highlighting the escalating nature of this crisis. You can learn more about these trends at Overdose Death Rates.
Florida has been significantly impacted by this crisis. Our state has seen a devastating rise in opioid-related fatalities, particularly those involving synthetic opioids like fentanyl. For those seeking resources and support within Florida, Florida’s State Opioid Response Project Resources offers valuable information.
Both illicit and prescription opioids contribute to the crisis. While much of the early attention focused on prescription painkillers, the landscape has shifted, with illicitly manufactured opioids now driving a significant portion of overdose deaths.
Types of Opioids and Their Potency
Opioids are a diverse class of drugs, all acting on the brain’s opioid receptors, but varying in their origin and strength:
- Natural Opioids (Opiates):
- Morphine: A powerful pain reliever, often used in hospital settings.
- Codeine: A weaker opioid, commonly found in some prescription cough syrups and pain medications.
- Semi-Synthetic Opioids:
- Heroin: An illicit, highly addictive opioid.
- Oxycodone (e.g., OxyContin, Percocet): A potent prescription painkiller.
- Hydrocodone (e.g., Vicodin, Norco): Another widely prescribed pain medication.
- Synthetic Opioids:
- Fentanyl: A highly potent synthetic opioid, often prescribed for severe pain but also widely produced illicitly.
- Carfentanil: An analog of fentanyl, used as an elephant tranquilizer, and incredibly dangerous to humans, with potency exponentially higher than fentanyl. As we’ve seen, Carfentanil: Elephant sedative killing people highlights its extreme risks.
The potency of these substances is a critical factor in overdose risk. Fentanyl, for instance, is about 50 times more potent than heroin and 100 times more potent than morphine. You can find more detailed information on these substances in the Drugs of Abuse: A DEA Resource Guide (.pdf).
The Role of Fentanyl in the Current Crisis
Fentanyl is at the epicenter of the current opioid use disorder and overdose crisis, particularly here in Florida. Its extreme potency is a major contributor to the alarming rise in overdose deaths.
While pharmaceutical fentanyl is legally prescribed for severe pain, the vast majority of fentanyl-related deaths now involve illicitly manufactured fentanyl (IMF). This IMF is often pressed into counterfeit pills designed to look like legitimate prescription medications (like Oxycodone or Xanax) or mixed into other illicit drugs such as heroin, cocaine, or methamphetamine, often without the user’s knowledge.
A tiny amount of fentanyl, invisible to the naked eye, can be lethal. The risk of accidental overdose is incredibly high because users have no way of knowing how much fentanyl is in their drugs, or if it’s present at all. Furthermore, the presence of substances like xylazine, a non-opioid sedative, in illicit fentanyl supplies can make overdoses even harder to reverse with naloxone.
For people in Miami and across South Florida who are struggling with fentanyl use, immediate and specialized help is crucial. At Summer House Detox Center, we understand the unique challenges of fentanyl withdrawal and offer Top-rated fentanyl detox at Summer House Detox Center in Miami, providing a safe and medically supervised pathway to recovery.
Pathways to Recovery: Effective Treatment for Opioid Use Disorder
The journey to overcome opioid use disorder is challenging, but it is unequivocally possible. The primary goals of treatment are to prevent overdose deaths, help individuals regain their health and social function, and support them in achieving long-term recovery. This requires a comprehensive, individualized approach that addresses both the physical and psychological aspects of OUD. Finding quality treatment is the first step, and resources like Finding Quality Treatment for Substance Use Disorders can guide you.
The First Step: Managing Opioid Withdrawal
For many, the fear of withdrawal is a major barrier to seeking help. Opioid withdrawal can be uncomfortable, but it’s a necessary first step in the recovery process. The symptoms can range from mild to severe, including:
- Intense cravings for opioids
- Muscle aches and bone pain
- Restlessness and insomnia
- Diarrhea, nausea, and vomiting
- Cold flashes with goosebumps (“cold turkey”)
- Involuntary leg movements
The timeline of withdrawal varies depending on the type of opioid used. For short-acting opioids like heroin, symptoms can begin within 6-12 hours of the last dose, peak around 24-72 hours, and subside within a week. For longer-acting opioids like methadone, withdrawal can start 2-3 days after the last dose and last for several weeks. You can learn more about specific symptoms and their duration at Opiate Withdrawal Symptoms.
While opioid withdrawal is rarely life-threatening on its own (unlike withdrawal from alcohol or benzodiazepines), its severity often drives individuals to continue using to avoid the excruciating discomfort. Quitting “cold turkey” without medical supervision is not only incredibly difficult but also significantly increases the risk of relapse and subsequent overdose, as tolerance decreases rapidly. This is why Why medical detox is a vital first step in recovery is so important.
At Summer House Detox Center in Miami, FL, we specialize in medically supervised detox programs, providing a safe and comfortable environment where withdrawal symptoms are managed with medication and expert care. Our dedicated Opiate Detox Center in Miami, FL ensures that individuals move through this challenging phase with dignity and support, setting a solid foundation for long-term recovery.
Medication-Assisted Treatment (MAT) for Opioid Use Disorder
Medication-Assisted Treatment (MAT) is considered the gold standard for treating opioid use disorder. It’s an evidence-based approach that combines FDA-approved medications with counseling and behavioral therapies. This comprehensive strategy addresses the whole person, not just the substance use. You can explore more about this approach at Medication-Assisted Treatment (MAT).
MAT medications help to:
- Normalize brain chemistry and reduce the intense physiological drive to use
- Relieve cravings that often lead to relapse
- Prevent withdrawal symptoms, allowing individuals to focus on therapy and recovery
- Block opioid effects, making it less rewarding to use illicit substances
Research shows these treatments are highly effective and can greatly reduce the use of illicit opioids and the risk of overdose. For more detailed information, see How effective are medications to treat opioid use disorder?.
A significant development in expanding access to MAT occurred with the MAT Act of 2022. This legislation eliminated the DATA-Waiver (X-Waiver) program, which previously required special training for healthcare providers to prescribe buprenorphine. Now, all DEA-registered practitioners with Schedule III prescribing authority can prescribe buprenorphine for OUD, making this vital medication more accessible to individuals in need, including those in Florida.
At Summer House Detox Center, we firmly believe in the power of MAT. Our Medication-Assisted Treatment services at Summer House Detox Center in Miami are custom to each individual’s needs, providing the medical support necessary for a successful recovery journey.
FDA-Approved Medications for OUD
There are three FDA-approved medications for treating opioid use disorder, each with a distinct mechanism of action and usage protocol. We can discuss these options with you at Summer House Detox Center to determine the best fit for your recovery journey in Miami, FL.
- Methadone: A long-acting opioid agonist that prevents withdrawal and reduces cravings. It’s dispensed daily at licensed clinics. Learn more about Methadone.
- Buprenorphine (Suboxone, Subutex): A partial opioid agonist that eases withdrawal and cravings without producing a strong high. It can be prescribed by certified doctors and taken at home. Learn more about Buprenorphine.
- Naltrexone (Vivitrol): An opioid antagonist that blocks the effects of opioids. It’s not an opioid, has no potential for abuse, and is not addictive. It’s usually started after a person has fully detoxed. Learn more about Naltrexone.
Choosing the right medication depends on individual needs, medical history, and treatment goals. For a detailed comparison, see Methadone vs Suboxone: How do they differ?.
The Role of Therapy and Treatment Settings at Summer House Detox Center
Medication is a crucial component, but it’s most effective when combined with behavioral therapies and counseling. These therapies help individuals address the root causes of their addiction, develop coping skills, and build a foundation for long-term recovery.
Key Therapeutic Approaches:
- Cognitive Behavioral Therapy (CBT): Helps patients recognize and change negative thinking patterns and behaviors associated with drug use.
- Contingency Management (CM): Uses positive reinforcement to encourage abstinence.
- Motivational Interviewing (MI): Helps individuals resolve ambivalence and find the internal motivation to change.
Treatment Settings at Summer House Detox Center:
- Detoxification (Detox): The first step, providing medical supervision to manage withdrawal symptoms safely. Our Drug and alcohol detox in Miami, FL offers a supportive environment for this critical phase.
- Inpatient/Residential Detox Stay: Provides intensive, 24-hour care in a structured, comfortable environment at our Miami facility.
After completing detox at Summer House Detox Center, many patients transition to community-based outpatient programs and mutual-help groups such as Narcotics Anonymous, which support long-term recovery for people living in Miami and throughout South Florida.
