Why Understanding Alcohol Withdrawal Matters for Your Recovery
Alcohol dependence symptoms withdrawal can be one of the most challenging and dangerous obstacles on the path to sobriety. If you’re reading this, you or someone you care about may be facing the difficult decision to stop drinking—and wondering what comes next.
Quick Answer: Key Alcohol Withdrawal Symptoms to Recognize
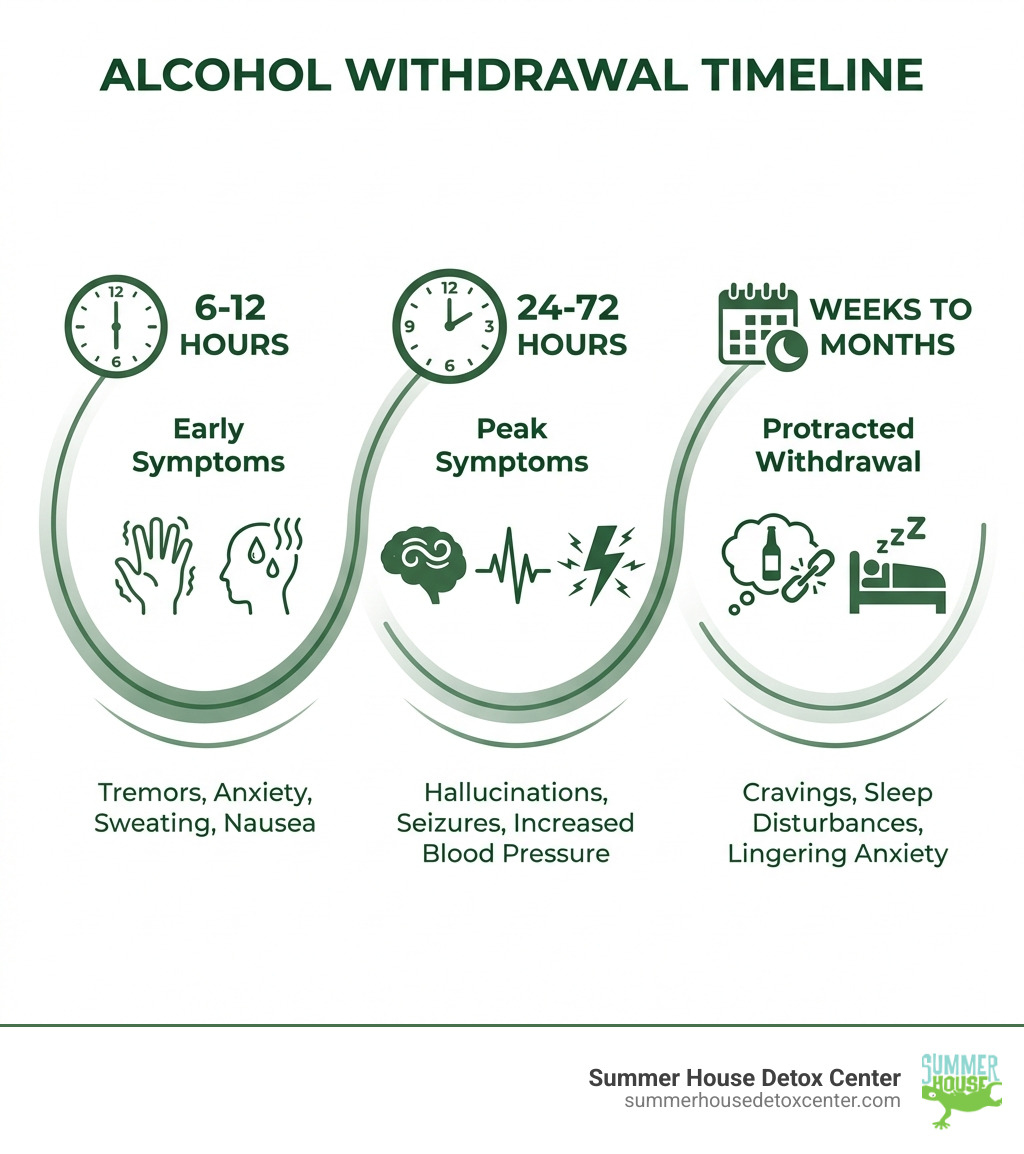
Withdrawal symptoms typically begin 6-12 hours after your last drink and vary in severity:
- Early Symptoms (6-12 hours): Tremors, anxiety, sweating, nausea, headache, insomnia
- Peak Symptoms (24-72 hours): Increased blood pressure, rapid heartbeat, hallucinations, seizures
- Severe Symptoms: Delirium tremens (DTs), confusion, high fever, life-threatening complications
- Protracted Symptoms (weeks to months): Lingering anxiety, sleep disturbances, cravings, irritability
Risk Factors for Severe Withdrawal: Heavy daily drinking (6+ drinks), long-term dependence, history of previous withdrawals, older age, co-occurring health conditions
More than half of Americans aged 18 and older—over 131 million people—drink alcohol. And in 2021, nearly a quarter met the criteria for an alcohol use disorder. Here in Florida and Miami, countless individuals struggle with the fear of withdrawal symptoms—often suffering through multiple failed attempts at quitting on their own.
The truth is, alcohol withdrawal is not just uncomfortable—it can be deadly. Approximately 5-10% of heavy alcohol users who experience severe withdrawal develop delirium tremens, which carries a mortality rate of up to 5% even with treatment. But here’s the hopeful news: medically supervised detox makes withdrawal safer, more comfortable, and sets the foundation for lasting recovery.
Understanding what happens during withdrawal—and why professional help is crucial—can be the difference between another failed attempt and a successful journey to sobriety. You don’t have to face this alone, and you deserve compassionate, expert care during this vulnerable time.
Alcohol dependence symptoms withdrawal glossary:
The Alcohol Withdrawal Timeline: What to Expect
When someone who is physically dependent on alcohol suddenly stops or significantly reduces their intake, their body and brain go into overdrive. This reaction is known as the alcohol withdrawal syndrome. Alcohol, a central nervous system depressant, slows down brain activity. To compensate for this constant suppression, the brain adapts by increasing excitatory neurotransmitter activity and decreasing inhibitory neurotransmission. When alcohol is removed, the brain is left in a state of hyperexcitability, leading to a cascade of symptoms that can range from uncomfortable to life-threatening. This state manifests as widespread autonomic hyperactivity and central nervous system (CNS) hyperexcitability.
Understanding the typical time course of these symptoms is crucial for recognizing alcohol dependence symptoms withdrawal and seeking appropriate care. While the exact timing and severity can vary greatly among individuals, a general pattern emerges, as outlined in guidance such as the Canadian Guidance on Alcohol and Health.

Stage 1: The First 6-12 Hours
For many, the first signs of withdrawal can begin surprisingly quickly—as early as six to twelve hours after their last drink. These early symptoms are often mild and might even be mistaken for a bad hangover, but they are a clear indication that the body is reacting to the absence of alcohol.
Common symptoms during this initial phase include:
- Tremors (shakes): Often noticeable in the hands, this is one of the most reliable physical signs of alcohol withdrawal.
- Anxiety: A feeling of nervousness, unease, or panic.
- Nausea and/or vomiting: Gastrointestinal distress is common.
- Headache: A throbbing or persistent pain in the head.
- Sweating: Excessive perspiration, even in cool environments.
- Insomnia: Difficulty falling or staying asleep.
These symptoms arise as the brain begins to rebound from alcohol’s depressant effects. While uncomfortable, medical supervision during this stage can help manage these symptoms and prevent them from escalating. For more detailed information on what to expect, you can explore our resources on detox timelines.
Stage 2: The Peak at 24-72 Hours
As the withdrawal progresses, symptoms typically intensify, reaching their peak severity between 24 and 72 hours after the last drink. This is often the most critical and dangerous period of alcohol withdrawal, as the central nervous system’s hyperexcitability can lead to more severe manifestations.
During this phase, individuals may experience:
- Increased blood pressure and rapid heartbeat: These are signs of significant autonomic hyperactivity.
- Hallucinations: These can be auditory (hearing things that aren’t there), visual (seeing things like crawling insects or shadows), or tactile (feeling sensations on the skin). Alcohol hallucinosis typically begins within 12 to 24 hours and may last up to two days.
- Seizures: Alcohol withdrawal seizures can occur anywhere from six to 48 hours after the last drink, with the risk peaking around 24 hours. These can be grand mal seizures and are a serious medical emergency.
- Delirium Tremens (DTs): The most severe form of alcohol withdrawal, DTs usually begin two to three days after the last drink, though they can be delayed for more than a week. Its peak intensity is often observed four to five days after cessation.
The risk of these severe symptoms underscores the critical importance of medical supervision. As highlighted in comprehensive reviews like the Alcohol Dependence, Withdrawal, and Relapse review, these phenomena are a direct consequence of the profound neurobiological changes induced by chronic alcohol exposure.
Stage 3: Post-Acute and Protracted Withdrawal
Even after the acute physical symptoms subside, the journey isn’t over. Many individuals experience what is known as Post-Acute Withdrawal Syndrome (PAWS), where lingering psychological and emotional symptoms can persist for weeks or even months. This subacute withdrawal syndrome is a significant factor in relapse.
Key characteristics of PAWS include:
- Dysphoria: A general state of unease or dissatisfaction, often manifesting as profound sadness or emotional numbness.
- Irritability and agitation: Heightened frustration and restlessness.
- Sleep disturbances: Persistent insomnia or disrupted sleep patterns.
- Cravings: Intense urges to consume alcohol, often triggered by stress, environmental cues, or emotional states.
These protracted symptoms can be incredibly challenging and contribute significantly to the motivation for relapse. Without ongoing support and coping strategies, the risk of returning to alcohol use remains high during this vulnerable period.
Understanding the Spectrum of Alcohol Dependence Symptoms Withdrawal
The severity of alcohol dependence symptoms withdrawal is not uniform; it exists on a spectrum from mild discomfort to life-threatening emergencies. Several factors influence where an individual falls on this spectrum, making personalized care essential, especially in a professional detox setting like ours in Miami.
Key risk factors that increase an individual’s likelihood of experiencing severe withdrawal include:
- Amount and duration of alcohol consumed: Generally, the more alcohol consumed daily and the longer the period of heavy drinking, the more severe the withdrawal symptoms are likely to be. However, it’s important to note that withdrawal requiring treatment is rare in people consuming fewer than six drinks per day, except in older adults.
- Previous detoxifications: A history of prior withdrawal episodes, particularly those involving seizures or delirium tremens, is a significant predictor of more severe future withdrawals. This phenomenon is known as “kindling” (which we’ll discuss further).
- Age and health status: Older adults may develop significant withdrawal symptoms even with lower daily alcohol consumption due to age-related physiological changes. Co-occurring medical conditions (such as infections, trauma, or liver disease) and poor general health can also exacerbate withdrawal severity.
- Co-occurring mental health conditions: Individuals with underlying anxiety disorders, depression, or other mental health challenges may experience more intense psychological withdrawal symptoms, and these conditions can complicate both the withdrawal process and long-term recovery.
- Nutritional deficiencies: Chronic alcohol abuse often leads to deficiencies in essential vitamins and minerals (e.g., thiamine, folate, magnesium), which can worsen neurological symptoms and increase the risk of complications like Wernicke-Korsakoff syndrome.
Understanding these individual risk factors allows us to tailor our treatment approach to each person’s unique needs. Learn more about our comprehensive treatment approach.
Reliable Physical and Psychological Symptoms
Recognizing the specific signs of alcohol withdrawal is paramount for timely intervention. While some symptoms can be subtle, others are quite pronounced.
Common physical signs of alcohol withdrawal include:
- Tachycardia: A rapid heart rate.
- Hypertension: Liftd blood pressure.
- Tremor: Shaking, particularly of the hands, which can be postural (when holding a position) or intention (when performing a task). This is considered the most reliable physical sign.
- Diaphoresis (excessive sweating): Often accompanied by clammy skin.
- Nausea and vomiting.
- Headaches.
Alongside the physical manifestations, significant psychological signs are prevalent:
- Agitation and restlessness: A feeling of unease and inability to relax.
- Anxiety: Often profound and distressing.
- Irritability: Short temper and heightened emotional reactivity.
- Sleep disturbances: Ranging from difficulty falling asleep to vivid, disturbing nightmares.
- Dysphoria.
These symptoms, both physical and psychological, collectively signal that the body is struggling to adapt to the absence of alcohol.

Distinguishing Withdrawal Anxiety from an Anxiety Disorder
Anxiety is a prominent feature of alcohol withdrawal, but it’s important for healthcare providers to distinguish this from a pre-existing or generalized anxiety disorder. While there can be overlapping features, key differences help in diagnosis and treatment planning.
| Feature | Alcohol Withdrawal Anxiety | Generalized Anxiety Disorder (GAD) |
|---|---|---|
| Symptom Onset | Develops rapidly after cessation or reduction of heavy alcohol use | Chronic, persistent, and not directly tied to substance withdrawal |
| Timing | Peaks within 24-72 hours, then gradually subsides (though can linger) | Persistent for at least 6 months, often lifelong |
| Physical Signs | Accompanied by other physical withdrawal signs (tremor, sweating, tachycardia) | May have physical symptoms (muscle tension, fatigue), but not specific withdrawal signs |
| Response to Alcohol | Symptoms are quickly relieved by consuming alcohol (a dangerous cycle) | Alcohol may be used as a coping mechanism, but doesn’t “cure” the underlying anxiety |
| History | Often linked to a history of heavy drinking, predictable morning/afternoon drinking | May have a family history, but not necessarily linked to alcohol abuse |
In Florida, where many individuals seek help for co-occurring mental health and substance use disorders, careful differentiation is vital. If a patient presents with anxiety, and also reports consuming six or more drinks per day (or even lower amounts for older adults), experiences sweating or tremor, or finds their anxiety relieved by alcohol, then alcohol withdrawal should be strongly suspected. Treating both the addiction and any underlying mental health conditions (dual diagnosis) is a cornerstone of effective recovery.
Severe Symptoms: When to Seek Emergency Help in Miami
While mild to moderate withdrawal can be managed with professional medical oversight, certain severe alcohol dependence symptoms withdrawal require immediate emergency medical attention. These symptoms indicate a high risk of life-threatening complications.
The most dangerous manifestation is Delirium Tremens (DTs). This severe form of withdrawal typically presents with:
- Profound confusion and disorientation: Inability to recognize time, place, or people.
- Severe agitation: Extreme restlessness and distress.
- High fever: Significant elevation in body temperature.
- Grand mal seizures: Uncontrolled electrical activity in the brain.
- Hallucinations: Often vivid and disturbing, leading to extreme fear.
- Rapid heart rate and liftd blood pressure.
DTs is a medical emergency. Historically, it had a mortality rate as high as 20%, though with modern critical care, prompt diagnosis, and treatment, this rate has significantly decreased to around 1-4%. If you or someone you know in Miami or anywhere in Florida exhibits these symptoms, do not hesitate to seek emergency medical care immediately. As noted in The alcohol withdrawal syndrome overview, these severe reactions are a critical concern.
The Vicious Cycle: How Withdrawal Fuels Dependence and Relapse
Understanding alcohol dependence symptoms withdrawal isn’t just about listing symptoms; it’s about grasping the insidious cycle that perpetuates addiction. Chronic alcohol use fundamentally alters brain chemistry, creating a vicious cycle where withdrawal symptoms drive continued drinking, making it incredibly difficult to break free.
At the heart of this cycle lies the neurobiology of addiction. Alcohol initially activates the brain’s reward system, releasing feel-good chemicals like dopamine. Over time, however, the brain adapts, leading to an “allostatic” state. This means the body’s physiological systems adjust to the chronic presence of alcohol, establishing a new, dysfunctional equilibrium. When alcohol is removed, these dysregulated systems, particularly those involved in reward and stress, are thrown into chaos. The intense discomfort of withdrawal then acts as a powerful negative reinforcement, driving the individual to drink again to alleviate the pain, thus fueling the cycle of dependence.
The Brain on Withdrawal: A State of Hyperexcitability
To truly understand alcohol dependence symptoms withdrawal, we need a glimpse into the brain’s delicate balance. Alcohol’s primary action is to improve the activity of gamma-aminobutyric acid (GABA), the brain’s main inhibitory neurotransmitter, and to suppress the activity of glutamate, the main excitatory neurotransmitter. This dual action leads to the sedative and relaxing effects of alcohol.
With chronic, heavy drinking, the brain attempts to maintain homeostasis. It compensates by downregulating GABA receptors (making them less sensitive to GABA) and upregulating N-methyl-D-aspartate (NMDA) receptors, a type of glutamate receptor (making them more sensitive to glutamate). When alcohol is suddenly removed, the brain is left with an overactive excitatory system and an underactive inhibitory system—a state of profound hyperexcitability. This imbalance manifests as the tremors, anxiety, seizures, and other severe symptoms characteristic of withdrawal. This critical neurobiological shift is a key reason why self-detox can be so dangerous. We also know that the stress response system, particularly involving corticotropin-releasing factor (CRF), plays a key role in alcohol dependence and withdrawal anxiety.
The “Kindling Effect”: Why Subsequent Withdrawals Are Worse
One of the most alarming aspects of alcohol withdrawal is a phenomenon known as the “kindling effect.” This refers to the observation that repeated episodes of alcohol withdrawal lead to progressively more severe withdrawal symptoms, even if the amount of alcohol consumed is not increasing. It’s as if each withdrawal “kindles” or sensitizes the brain, making it more prone to extreme reactions in subsequent withdrawals.
Research, including animal models such as those detailed in the animal model of alcohol withdrawal “kindling”, has shown that this sensitization results in:
- Increased severity of withdrawal with each cycle: Symptoms become more intense and appear more rapidly.
- Lower seizure threshold: The brain becomes more susceptible to seizures with less provocation.
- Increased relapse vulnerability: The heightened distress and discomfort of withdrawal drive a stronger urge to drink, making relapse more likely.
This means that someone who has gone through withdrawal multiple times is at a significantly higher risk for developing severe, life-threatening symptoms like seizures and delirium tremens during their next attempt at sobriety. This escalating risk underscores the urgency of seeking professional, medically supervised detox at facilities like Summer House Detox Center in Miami, where we understand this complex phenomenon.
The Role of Stress and Anxiety in Relapse
Stress and anxiety are not just symptoms of alcohol withdrawal; they are powerful drivers in the entire cycle of alcohol dependence, withdrawal, and relapse. The brain’s stress system, particularly the corticotropin-releasing factor (CRF) system, becomes dysregulated with chronic alcohol use.
During withdrawal, and even into protracted abstinence, individuals often experience heightened levels of anxiety and dysphoria. This persistent negative emotional state, amplified by a hyperactive stress system, creates a strong motivation to seek relief—and for someone with alcohol dependence, alcohol has historically been the most effective, albeit destructive, coping mechanism. This stress-induced craving is a significant predictor of relapse, as evidenced in studies on stress-induced craving in abstinent individuals.
The cycle looks like this: chronic drinking leads to physiological dependence. Stopping drinking causes withdrawal, including intense anxiety and stress. This anxiety and stress, in turn, triggers powerful cravings, leading to relapse, which then restarts the cycle of dependence. Breaking this cycle requires not only managing acute withdrawal but also addressing the underlying mechanisms of stress and anxiety that drive continued alcohol seeking.
Medically Supervised Detox: A Safe Path to Recovery in Florida
Given the complexities and dangers of alcohol dependence symptoms withdrawal, attempting to detox alone is not only incredibly difficult but can be life-threatening. This is why medically supervised detox, especially in a specialized facility like Summer House Detox Center in Miami, Florida, is not just recommended, but often essential.
Our approach focuses on providing a safe, comfortable, and supportive environment where individuals can steer the challenging withdrawal process under the constant care of experienced medical professionals. We understand the unique needs of our community here in Florida and are committed to offering personalized care.
The importance of professional medical management cannot be overstated:
- Symptom monitoring: Our team continuously monitors vital signs and withdrawal symptoms, adjusting care as needed to ensure safety.
- Preventing severe complications: Medications and interventions are administered proactively to prevent the escalation of symptoms to seizures, delirium tremens, and other dangerous conditions.
- Comfort and dignity: We prioritize patient comfort and dignity throughout the detox process, minimizing distress and supporting emotional well-being.
- Creating a foundation for long-term recovery: Detox is the crucial first step. By safely clearing the body of alcohol, we prepare individuals for the next stages of treatment and therapy that address the underlying causes of addiction.
To learn more about our comprehensive detox services and how we can support you or a loved one, please visit our page on alcohol detox.
Pharmacological Treatments for Alcohol Dependence Symptoms Withdrawal
Pharmacological interventions are a cornerstone of safe and effective alcohol withdrawal management. These medications help to alleviate symptoms, prevent severe complications, and stabilize the patient during this critical period.
The primary class of medications used are benzodiazepines, such as lorazepam, diazepam, and chlordiazepoxide. These drugs work by enhancing GABA activity in the brain, counteracting the hyperexcitability caused by alcohol withdrawal. They effectively reduce anxiety, prevent seizures, and manage agitation. The dosing of benzodiazepines can follow two main strategies:
- Symptom-triggered dosing: Medications are given only when specific withdrawal symptoms reach a certain severity, as measured by assessment tools like the Clinical Institute Withdrawal Assessment for Alcohol, Revised (CIWA-Ar) scale. This approach often leads to lower total medication doses and shorter treatment durations.
- Fixed-dose schedules: Medications are given at regular intervals, with doses gradually tapered down over several days.
Research comparing effects of carbamazepine and lorazepam in withdrawal and other studies have shown that symptom-triggered regimens are generally preferred due to their efficacy and reduced medication exposure.
Other medications may also be used:
- Anticonvulsants: Drugs like gabapentin or carbamazepine may be used, particularly if benzodiazepines are contraindicated or to address specific symptoms like cravings or sleep disturbances.
- Nutritional support: Thiamine (vitamin B1) supplementation is critical to prevent Wernicke-Korsakoff syndrome, a serious neurological disorder associated with chronic alcohol abuse. Other vitamins and minerals, such as folate, magnesium, and potassium, are also often replenished.
Medications for Relapse Prevention
Once acute withdrawal is managed, the focus shifts to preventing relapse and supporting long-term sobriety. Several medications are approved to help individuals maintain abstinence by targeting the neurobiological pathways involved in craving and reward.
- Naltrexone: This medication works as an opioid receptor antagonist, meaning it blocks the euphoric and rewarding effects of alcohol. By doing so, it can reduce alcohol cravings and the pleasure derived from drinking, making relapse less appealing.
- Acamprosate: While its exact mechanism is not fully understood, acamprosate is thought to modulate glutamate neurotransmission, helping to restore the balance between excitatory and inhibitory systems in the brain that was disrupted by chronic alcohol use. It helps reduce post-acute withdrawal symptoms like anxiety and sleep disturbances.
- Disulfiram: This medication works differently by interfering with the metabolism of alcohol. If a person consumes alcohol while taking disulfiram, they will experience unpleasant physical reactions, such as nausea, vomiting, and flushing. This creates a strong deterrent to drinking.
The effectiveness of these medications is often improved when combined with behavioral therapies, as demonstrated in studies like The COMBINE study on combined therapies. These pharmacological tools, combined with comprehensive therapy and support, offer individuals a stronger chance at sustained recovery.
Conclusion
The journey through alcohol dependence symptoms withdrawal is undoubtedly one of the most formidable challenges an individual can face. We’ve explored the intricate timeline of symptoms, from early tremors and anxiety to the severe, life-threatening manifestations of seizures and delirium tremens. We’ve also digd into the underlying neurobiological changes, such as GABA and glutamate imbalance, and the dangerous “kindling effect,” where each withdrawal episode can worsen the next, making future attempts at sobriety even more perilous. Moreover, the pervasive influence of stress and anxiety acts as a constant threat, fueling cravings and increasing the risk of relapse.
The message is clear: attempting to steer alcohol withdrawal alone is a dangerous gamble. The physical and psychological toll is immense, and the risk of severe complications, including death, is very real.
But there is hope, and a path to recovery. Medically supervised detox offers a safe, compassionate, and effective way to manage withdrawal symptoms, prevent complications, and lay the groundwork for a healthier, alcohol-free life. At Summer House Detox Center in Miami, Florida, we are dedicated to providing personalized care that respects your dignity and supports your journey. Our experienced team understands the complexities of alcohol dependence and withdrawal, ensuring you receive the expert attention you deserve.
You don’t have to face this unseen struggle alone. We are here to help you reclaim your life from alcohol dependence. For a confidential conversation about your options and how we can support you, please contact us for a confidential consultation today.
