Understanding the Challenge of Benzodiazepine Dependence
How to manage benzo withdrawal safely requires medical supervision, gradual tapering, and comprehensive support. Here’s what you need to know:
Essential Steps for Managing Benzo Withdrawal:
- Never stop abruptly – Quitting “cold turkey” can cause life-threatening seizures
- Seek medical supervision – Professional oversight is critical for safety
- Follow a tapering schedule – Gradual dose reduction (typically 5-10% every 2-4 weeks)
- Consider inpatient detox – Especially if you’ve been taking high doses (>50mg diazepam equivalent) or have other health conditions
- Use supportive therapies – Counseling, stress management, and holistic care improve outcomes
- Plan for the long term – Withdrawal can take weeks to months; patience is key
Benzodiazepines like Xanax, Klonopin, and Valium are commonly prescribed for anxiety and insomnia. While effective short-term, these medications can lead to physical dependence after just a few weeks of regular use. If you’ve been taking benzos for months or years, your brain has adapted to their presence. Stopping suddenly isn’t just uncomfortable—it can be dangerous.
Benzodiazepine withdrawal syndrome is a serious medical condition that requires the same careful attention as withdrawal from alcohol. About 40% of patients who suddenly stop a long-acting benzodiazepine after six months or more of use experience withdrawal symptoms. For those on higher doses or shorter-acting benzos like Xanax, that number can be even higher.
The good news? With proper medical care, you can safely withdraw from benzodiazepines and reclaim your life. Here in Miami and throughout Florida, specialized detox centers like Summer House Detox Center offer the expertise and compassionate support you need to steer this challenging process.
This guide will walk you through what to expect during benzo withdrawal, why medical supervision is non-negotiable, and how a structured tapering plan can help you achieve lasting freedom from dependence.
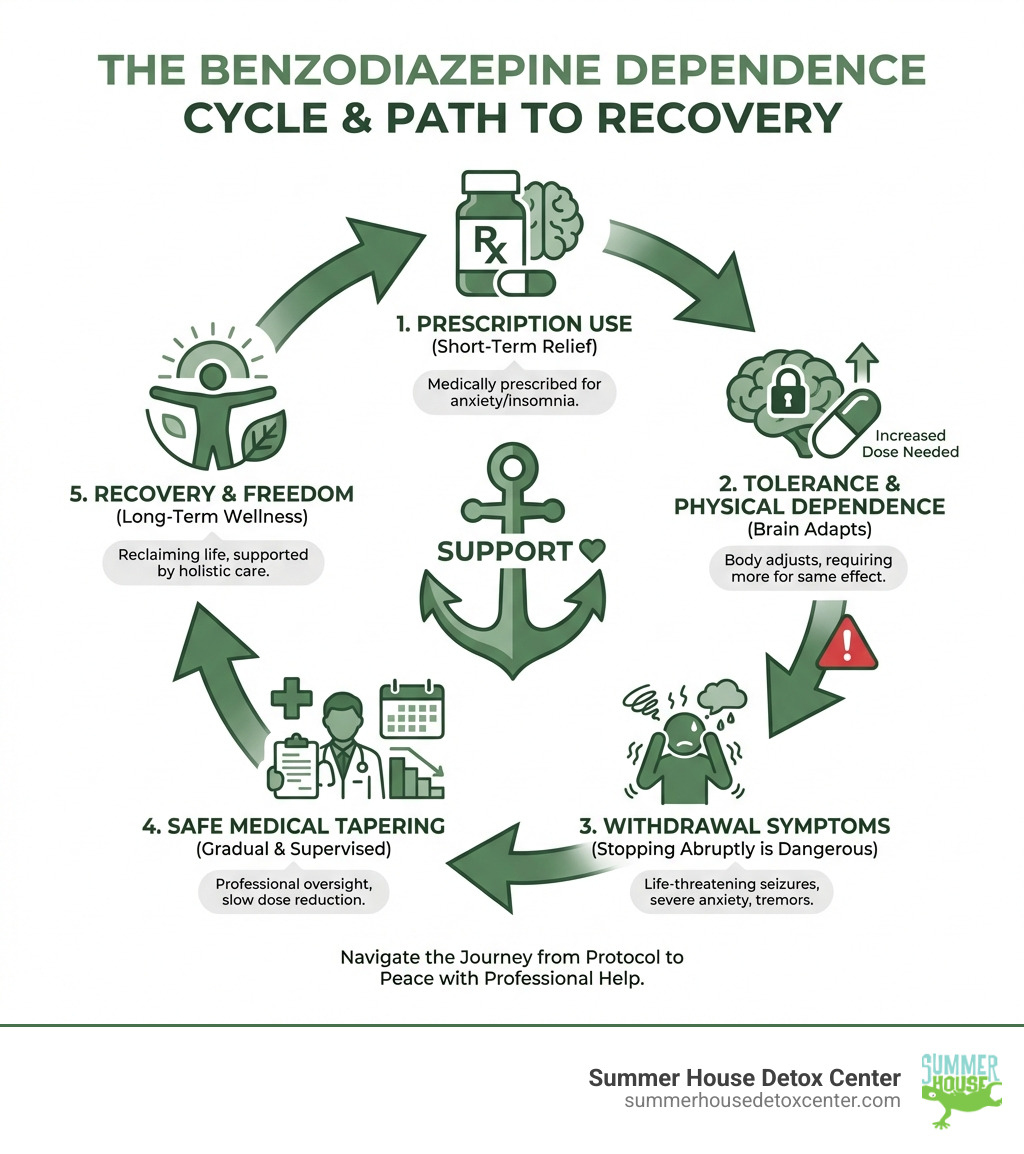
How to manage benzo withdrawal helpful reading:
Understanding Benzo Withdrawal: Symptoms, Phases, and Timeline
When someone becomes physically dependent on benzodiazepines, their brain and body adapt to the drug’s presence. Benzodiazepines work by enhancing the effects of gamma-aminobutyric acid (GABA), the brain’s primary inhibitory neurotransmitter. This slows down brain activity, producing calming effects. When the drug is reduced or stopped, the brain, now accustomed to this artificial calm, becomes overactive, leading to a cascade of uncomfortable and potentially dangerous withdrawal symptoms.
The symptoms of benzodiazepine withdrawal are diverse and can affect both the body and mind. Physically, individuals might experience nausea, tremors, sweating, headaches, heart palpitations, and muscle pain. More severely, seizures, muscle spasms, vomiting, diarrhea, blurred vision, and twitching can occur. Psychologically, withdrawal often manifests as heightened anxiety, panic attacks, depression, irritability, mood swings, agitation, and difficulties with concentration and memory. Some individuals may also experience perceptual distortions, such as hypersensitivity to noise, depersonalization, or even hallucinations and psychosis.
The timeline and severity of these symptoms are influenced by several factors, including the specific type of benzodiazepine used, the dosage, the duration of use, and whether other substances were also being used. Withdrawal symptoms typically begin within 24 hours of the last dose and can last from a few days to several months, or even years in some cases.

The Three Phases of Withdrawal
To better understand how to manage benzo withdrawal, it’s helpful to break down the process into distinct phases:
- Early Withdrawal: This phase typically begins hours to a few days after the last dose, depending on the benzodiazepine’s half-life. Symptoms often include a return of the original anxiety or insomnia that the medication was prescribed for, often with increased intensity (known as rebound symptoms). You might also start feeling general discomfort, restlessness, and mild physical symptoms.
- Acute Withdrawal: This is often the most challenging phase, lasting from a few days to several months. During acute withdrawal, symptoms peak in intensity. In addition to the symptoms mentioned above, individuals may experience more severe manifestations like seizures, panic attacks, extreme agitation, severe insomnia, gastrointestinal issues, and even psychosis. The intensity of these symptoms underscores why medical supervision is critical during this period.
- Protracted Withdrawal Syndrome (PAWS): For about 10% of people who stop taking benzodiazepines, withdrawal symptoms can persist for months or even years after the acute phase. This is known as Protracted Withdrawal Syndrome (PAWS). PAWS can involve lingering or intermittent symptoms such as persistent tinnitus, cognitive impairment (memory and concentration problems), chronic anxiety, depression, paresthesia (tingling or numbness), muscle pain, and sleep disturbances. While these symptoms typically lessen over time, they can be incredibly frustrating and debilitating, requiring ongoing support and management.
How the Type of Benzodiazepine Affects Withdrawal
The half-life of a benzodiazepine—how long it stays active in your system—significantly impacts the onset and intensity of withdrawal symptoms.
| Benzodiazepine Type | Examples | Half-Life (Approx.) | Onset of Withdrawal | Typical Withdrawal Intensity |
|---|---|---|---|---|
| Short-Acting | Alprazolam (Xanax) | 6-20 hours | 10-24 hours after last dose | More intense and rapid |
| Lorazepam (Ativan) | 10-20 hours | 1-2 days after last dose | Moderately intense | |
| Long-Acting | Diazepam (Valium) | 20-100 hours | 1-7 days after last dose | Less intense, but prolonged |
| Clonazepam (Klonopin) | 18-50 hours | 2-7 days after last dose | Less intense, but prolonged |
Short-acting benzodiazepines, like Xanax (alprazolam), leave the body more quickly, leading to a faster onset of withdrawal symptoms (often within 10-12 hours) that can be more intense. This rapid drop can feel like hitting a brick wall. Conversely, longer-acting benzodiazepines, such as Valium (diazepam) or Klonopin (clonazepam), are cleared from the system more slowly. This means withdrawal symptoms might take longer to appear (sometimes a few days) and may be less acutely intense, but they can last for a longer duration. Understanding these differences helps us tailor the most effective tapering strategy for you.
The Dangers of Abrupt Discontinuation and Key Risk Factors
Attempting to quit benzodiazepines “cold turkey” is not only extremely uncomfortable but also incredibly dangerous. Abruptly stopping these medications, especially after prolonged or high-dose use, can lead to severe and life-threatening complications.

The most alarming risks of abrupt discontinuation include grand mal seizures, delirium, psychosis, and even coma. These severe reactions can be fatal if not medically managed. We’ve seen cases where individuals attempting to quit on their own have experienced such intense psychological distress, including suicidal ideation, that it becomes an immediate medical emergency. For example, one study reported that one-third of mothers who suddenly discontinued their benzodiazepines became acutely suicidal due to unbearable symptoms. This highlights why professional medical supervision is non-negotiable for anyone seeking to withdraw from benzos.
Who is Most at Risk for Severe Withdrawal?
Several factors can increase the likelihood or severity of benzodiazepine withdrawal symptoms:
- High-Dose Users: Individuals taking high doses, particularly those exceeding 50mg diazepam equivalent per day, are at a significantly higher risk for severe withdrawal. In such cases, inpatient management is often recommended.
- Long-Term Use: The longer someone has used benzodiazepines, the more dependent their body becomes. Dependence rates are much higher, at 20% to 45%, after more than a year of use. Even after six months of use, about 40% of patients who stop a long-acting benzodiazepine will experience withdrawal.
- Polydrug Use: Using benzodiazepines alongside other central nervous system depressants like opioids, gabapentinoids, alcohol, or even certain antidepressants (e.g., tricyclic antidepressants) dramatically increases the risk of severe and complicated withdrawal. This is a key reason why we prioritize medical supervision.
- Co-occurring Mental Health Disorders: Pre-existing mental health conditions, such as severe anxiety, panic disorder, or depression, can exacerbate withdrawal symptoms and make the process more challenging.
- The Elderly: Older adults are particularly vulnerable. Their bodies metabolize benzodiazepines more slowly, and they are at a higher risk of experiencing confusion, disorientation, delirium, and falls during withdrawal.
- History of Seizures: Anyone with a personal history of seizures faces an liftd risk of experiencing seizures during benzodiazepine withdrawal.
- Abrupt Cessation: As discussed, stopping abruptly is the single biggest risk factor for severe and dangerous withdrawal symptoms.
How to Manage Benzo Withdrawal: A Step-by-Step Guide
Successfully managing benzodiazepine withdrawal is a journey best undertaken with professional medical guidance. At Summer House Detox Center in Miami, Florida, we understand the complexities involved and provide a safe, supportive environment for this process.
The cornerstone of how to manage benzo withdrawal safely is medical supervision, with tapering as the gold standard. While outpatient tapering can be appropriate for some, inpatient detox often offers the safest and most comfortable option, especially for those at higher risk. Our team develops personalized treatment plans, ensuring your comfort and safety every step of the way.
The Gold Standard: Medically Supervised Tapering
Tapering involves gradually reducing the benzodiazepine dosage over time, allowing your brain and body to slowly adjust. This is a far safer approach than quitting cold turkey.
- Assessment and Stabilization: The first step is a thorough medical assessment. If you’re on a short-acting benzodiazepine, our medical team may recommend switching you to a longer-acting equivalent, like diazepam (Valium), which provides a smoother, more controlled reduction due to its longer half-life. We use established diazepam equivalent dose charts to ensure accurate conversion.
- Gradual Dose Reduction: Under the principles often outlined in resources like the Ashton Manual, we implement a slow, steady reduction schedule. Initial dose reductions typically range from 5% to 25% of the starting dose, with further reductions of 5% to 10% every one to four weeks, as tolerated. For outpatient settings, these tapers usually need to be slower than inpatient tapers, sometimes extending to several months or even a year for long-term users. The American Society of Addiction Medicine (ASAM) recommends reductions of 5-10% every 2-4 weeks, not exceeding 25% every two weeks.
- Flexibility is Key: Your tapering schedule is highly individualized. We monitor your response after each reduction. If withdrawal symptoms become too intense, we can pause the taper, stabilize your dose, and then resume at a slower pace once you’re more comfortable. The goal is to minimize discomfort, not to rush the process.
Supportive Care for a Smoother Taper
Beyond the tapering schedule, comprehensive supportive care is crucial for making your withdrawal as smooth as possible. At Summer House Detox Center, our medical staff provides 24/7 monitoring, ensuring immediate response to any acute symptoms.
- Symptom Management: We address physical discomforts like nausea, headaches, and muscle pain with appropriate medications. For anxiety and sleep disturbances, which are common during withdrawal, we focus on non-pharmacological approaches first, but may use adjunctive medications if necessary, avoiding those that could complicate withdrawal.
- Emotional Support: The psychological aspects of benzo withdrawal can be intense. Our compassionate team provides reassurance and emotional support, helping you understand that what you’re experiencing is a temporary, expected part of the healing process.
- Safety and Comfort: Our facility is designed to be a safe, calm, and comfortable environment, reducing external stressors that could exacerbate withdrawal symptoms. Your dignity and well-being are our top priorities.
Holistic and Non-Pharmacological Strategies for Recovery
How to manage benzo withdrawal effectively also means integrating holistic and non-pharmacological strategies that support your overall well-being and equip you with coping mechanisms for the long term. These therapies are an integral part of our personalized approach at Summer House Detox Center:
- Psychotherapy: Cognitive Behavioral Therapy (CBT) is highly effective in addressing underlying anxiety, depression, and thought patterns that may have contributed to benzodiazepine use. Our therapists work with you to develop healthy coping strategies. Learn more about our holistic detox services.
- Support Groups: Connecting with others who understand your struggles can be incredibly powerful. We facilitate support groups and peer support within our facility, fostering a sense of community and shared experience.
- Stress Management Techniques: We offer various techniques like yoga, meditation, and mindfulness exercises to help you regulate your nervous system, reduce anxiety, and promote relaxation.
- Lifestyle Adjustments: Proper nutrition and hydration are vital for healing your body and brain. We provide balanced meals and encourage adequate fluid intake. Gentle exercise, appropriate for your physical condition, can also improve mood and sleep. Establishing good sleep hygiene practices is also key to addressing withdrawal-related insomnia.
Choosing the Right Setting: Inpatient Detox at Summer House Detox Center
Deciding on the appropriate level of care for benzodiazepine withdrawal is a critical decision, with safety being our primary concern. For residents of Miami and across Florida, Summer House Detox Center offers a specialized inpatient setting designed for safe and effective withdrawal management.
When is Inpatient Detox Necessary?
While some individuals may be candidates for outpatient tapering, certain conditions necessitate the comprehensive care provided by an inpatient detox facility like ours:
- High-Dose Dependency: If you’ve been taking a high dose of benzodiazepines (e.g., over 50mg diazepam equivalent per day), the risks of severe withdrawal are significantly increased, making 24/7 medical supervision essential.
- Polydrug Abuse: When benzodiazepines are used in combination with other substances like opioids or alcohol, the withdrawal process becomes much more complex and dangerous. Polydrug dependence is a strong indicator for inpatient care.
- Co-existing Medical or Psychiatric Issues: Individuals with other major medical conditions or severe psychiatric disorders require constant medical oversight to manage both their withdrawal symptoms and their co-occurring health challenges.
- History of Severe Withdrawal: If you’ve previously attempted withdrawal and experienced severe symptoms (e.g., seizures, delirium), an inpatient setting provides the necessary safety net.
- Lack of a Stable Home Environment: A supportive, stable, and substance-free environment is crucial for successful withdrawal. If your home situation is not conducive to recovery, inpatient care offers a controlled and therapeutic setting.
The benefits of 24/7 medical monitoring in a facility like Summer House Detox Center cannot be overstated. We can quickly respond to complications, adjust medication as needed, and provide continuous emotional support, significantly improving safety and comfort.
How Summer House Detox Center Supports Your Recovery
At Summer House Detox Center in Miami, FL, we pride ourselves on offering a unique and effective approach to benzodiazepine withdrawal. Our dedicated team is committed to providing:
- Personalized Care Plans: We understand that every individual’s journey is unique. Our medical and therapeutic teams collaborate to create a customized withdrawal plan custom to your specific needs, history, and goals.
- Experienced Medical Staff: Our team includes doctors, nurses, and support staff, some of whom are in recovery themselves, offering both clinical expertise and empathetic understanding. We provide continuous medical monitoring and care.
- Holistic Therapies: Beyond medication management, we integrate a range of holistic therapies to nurture your mind, body, and spirit, promoting overall healing and well-being.
- Ongoing Support for Long-Term Recovery: Detox is just the first step. We help you connect with resources and develop strategies for continued sobriety and well-being post-detox, whether through our own programs or referrals to trusted partners in Florida.
- Safe, Comfortable Environment: Our facility offers a serene and private setting where you can focus solely on your healing, free from the triggers and stressors of your everyday life.
Frequently Asked Questions about Managing Benzo Withdrawal
We often hear similar questions from individuals and their loved ones about how to manage benzo withdrawal. Here are some common concerns:
How long does acute benzo withdrawal last?
The acute phase of benzodiazepine withdrawal typically lasts between two to four weeks. However, this can vary significantly based on the type of benzo, the dosage, how long it was used, and individual physiology. For some, especially those on long-acting benzos, acute symptoms might extend for several months.
Can you die from benzo withdrawal?
Yes, it is possible to die from benzodiazepine withdrawal, particularly if it’s attempted abruptly (“cold turkey”) without medical supervision. The most dangerous complications are grand mal seizures, which can lead to injury or death, and severe delirium or psychosis, which can result in accidents or suicidal ideation. This is precisely why medical supervision is not just recommended, but essential for safety.
What helps with anxiety during benzo withdrawal?
Anxiety is one of the most prominent and distressing symptoms during benzo withdrawal. While medication tapering helps, non-pharmacological strategies are crucial. These include mindfulness, deep breathing exercises, and cognitive-behavioral therapy (CBT), which can help reframe anxious thoughts. Engaging in support groups provides peer understanding and coping strategies. It’s also vital to avoid substances that can worsen anxiety, such as caffeine and other stimulants. At Summer House Detox Center, we integrate these approaches into our treatment plans to help manage anxiety effectively.
Conclusion: Your Path to a Benzo-Free Life Starts Here
Understanding how to manage benzo withdrawal is the first critical step toward reclaiming your health and well-being. We’ve learned that abruptly stopping benzodiazepines is dangerous and can lead to severe, even life-threatening, complications. The gold standard for safe withdrawal is a medically supervised, gradual tapering process, ideally in an inpatient setting for those at higher risk.
Recovery from benzodiazepine dependence is not just a possibility; it’s a reality we witness every day at Summer House Detox Center. We provide the expertise, compassionate care, and supportive environment needed to steer this challenging journey. If you’re in Miami or anywhere across Florida, and you’re ready to break free from benzodiazepine dependence, we are here to help. Your journey to a peaceful, benzo-free life starts with reaching out for professional support.
Start your recovery journey with a confidential consultation.
